IRWG seed grant supports first-of-its-kind mHealth app for teen girls


by Laura Bailey
As a clinical psychologist working with high-risk populations, Golfo Tzilos Wernette often listened to her young female patients’ concerns about pressure to have unprotected sex—especially if alcohol was involved. This population also has the highest rates of several sexually transmitted infections, which now hover at record levels overall.
Tzilos Wernette, an assistant professor in the Departments of Family Medicine and Psychiatry, hopes to help these women prevent STIs by developing the first known mobile app tailored for adolescent girls at risk for substance use and sexual risk taking. Girls could educate themselves privately, or turn to their phones for in-the-moment answers and support.
To that end, Tzilos Wernette and her research team used her IRWG seed grant to fund a pilot study of in-person interviews and online surveys with high-risk young women, to better understand if they wanted information about sexual health and alcohol use and how they’d use it, and the most helpful content and how to deliver it.
The teens embraced the idea—87 percent of online respondents said they’d use a mHealth app, and the interviews yielded some surprising themes. Tzilos Wernette learned that the girls—ages 15 though 19 and old enough for sex education classes—knew very little about STIs or their own STI risk.
“They were much more concerned about pregnancy,” Tzilos Wernette said. “This surprised me. I think there’s been such effort to reduce teen pregnancy over the years, which is a great outcome, but we are falling short with information for adolescents about STIs, so they have a sense of invincibility.”
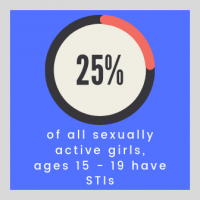
But they aren’t invincible—and the statistics are ugly. Research suggests that 25 percent of all sexually active girls age 15 through 19 have STIs, with chlamydia and gonorrhea rates highest among this age group. STIs are associated with significant morbidity and mortality, including premature death. Women are biologically more susceptible to STIs, and the combination of peer pressure, male-female power imbalances, and alcohol, make negotiating condom use tough.
“We’re trying to develop approaches to give them facts and also to empower them,” said Tzilos Wernette.
This population lacks STI information for several reasons. A majority of women don’t receive the CDC-recommended STI screens because they’re too afraid to disclose risky sexual behavior to physicians, or, they simply don’t understand their risk enough to ask.
Tzilos Wernette said that this naivete was evident throughout the interviews. For instance, many women said they trusted their partners to disclose an STI, or deemed their partner “too young” for STIs.
The good news is that research shows that mHealth apps reduce alcohol use and increase STI testing among this age group. The 2015 Pew Teens & Technology Surveys found 88% of youth report having cell phones (73% are smartphones), so this app could cast a wide net.
The women surveyed said they wanted something that wouldn’t shame them, with detailed information on STIs, coercion and sexual assault and prevention, and safe alcohol use without scare tactics or abstinence messages.
“Studies show that adolescents who perceive they are at risk for STIs engage in less risky behavior,” Tzilos Wernette said. “The beauty of using an app is that it is a potentially low-cost way that we can reach more adolescents, providing greater impact.”
Tzilos Wernette’s collaborator, Rob Stephenson, professor in the School of Nursing and director of the Center for Sexuality and Health Disparities, has developed numerous mHealth youth applications, and they plan to adapt this existing technology.
The findings were presented at the Research Society on Alcoholism (RSA) annual meeting in June. A manuscript is underway and soon, researchers will submit for federal grant funding to develop the mobile app.
“As researchers, we read these recommendations, for example, the World Health Organization has made STI prevention one of its top priorities,” Tzilos Wernette said. “We hope that efforts can line up with those recommendations, and that there is funding available. We don’t want to shortchange individuals who are at risk. We want to fund work to improve their lives and their health outcomes.”
The IRWG Faculty Seed Grant program, established in 1996, supports disciplinary and interdisciplinary faculty projects on women, gender and sexuality. Learn more about this program and view upcoming opportunities.
